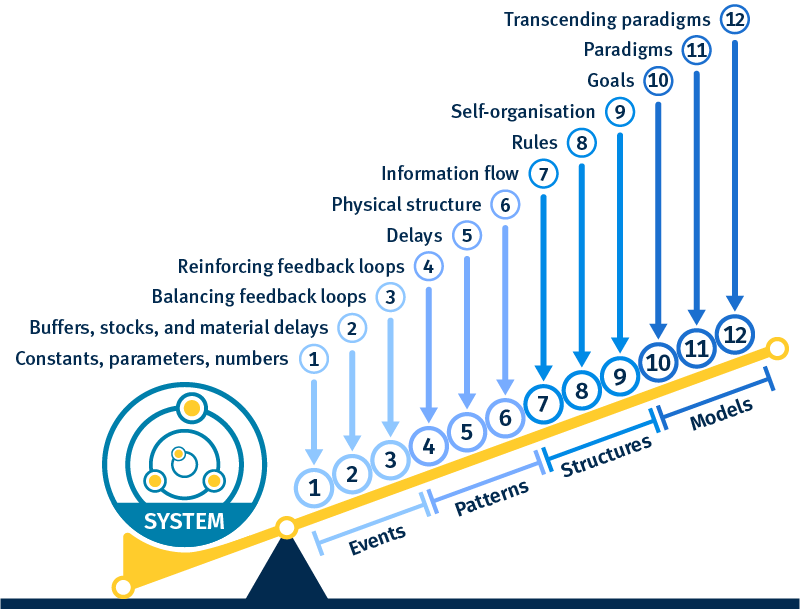
When moving from a problem synthesis to action, there are many places you can target to ‘leverage’ change.
Donella Meadows, an early systems thinking leader identified 12 leverage points or strategic ‘places to intervene’ where small shifts can bring about big changes.
The leverage points are listed in increasing order of leverage. While high leverage points represent enticing opportunities, they are harder to shift like the deeper layers of the iceberg model.
- Events
- Patterns
- Structures
- Models
Events
1. Constants, parameters, numbers
Numerical values that determine how a system behaves.
E.g. Adjusting the number of staff in an ICU to optimise patient care.
2. Buffers, stocks, and material delays
Systems elements that store resources or information.
E.g. Increasing the stock of essential medications to prevent shortages.
3. Balancing feedback loops
Feedback loops that maintain equilibrium in a system.
E.g. Implementing a system to monitor and adjust staffing levels, based on patient acuity, to maintain quality of care.
Patterns
4. Reinforcing feedback loops
Feedback loops that amplify change within a system.
E.g. Reduced waitlists for an outpatient clinic results in improved referrer satisfaction, resulting in increased referrals.
5. Delays
Delays in how a system responds to change.
E.g. Reducing the time between a patient's admission and the start of treatment to improve outcomes.
6. Physical structure
The physical layout or design of a system.
E.g. Redesigning the layout of a clinic to improve patient flow and reduce waiting times.
Structures
7. Information flow
How information is communicated within a system.
E.g. Implementing a well-designed digital system for sharing patient records to improve coordination of care.
8. Rules
The governing rules and regulations that dictate how a system operates.
E.g. Implementing guidelines for hand hygiene to reduce healthcare-associated infections.
9. Self-organisation
The ability of a system to organise itself without external intervention.
E.g. Allowing teams to self-organise their schedules to improve workflow efficiency.
Models
10. Goals
Objectives that drive the behaviour of a system.
E.g. Setting a goal to improve equity of access to care and supporting strategies to achieve this goal.
11. Paradigms
The underlying beliefs and assumptions that shape how a system is understood and managed.
E.g. Shifting from a reactive approach to healthcare to a proactive, preventive care model.
12. Transcending paradigms
Changing the fundamental mindset or worldview that underlies a system.
E.g. Embracing a patient-centered care approach that considers patients' values and preferences in treatment decisions.